From left to right: Drs. Kathleen Berfield, Lara Oyetunji and Tori Lennox.
Lara Oyetunji, MD, MPH is a cardiothoracic surgeon who specializes in the treatment of all adult general cardiac surgical diseases. She serves as the section chief of Cardiac Surgery at the Veterans Administration Puget Sound and also sees patients at the UW Medical Center – Montlake campus.
Oyetunji’s clinical interests include surgical and transcatheter approaches to the management of valvular heart diseases including aortic stenosis, mitral valve disease and hypertrophic cardiomyopathy. She has a keen interest in global surgery and seeks to develop academic partnerships toward sustainable surgical programs in low- and middle-income countries.
Oyetunji took a moment to sit down and speak with us about her journey as a student from Nigeria to section chief of cardiac surgery at the Puget Sound VA hospital in Seattle — and how her experiences shaped her goals.
When did you know you wanted to become a doctor?
I had surgery at the age of 10 and, instead of trepidation, I vividly remember a sense of excitement and intrigue while being inside the operating room. After completing high school in Nigeria, my parents opted to send my siblings and me to the U.S. for higher education. It must have been a tough decision to send their 17-year-old daughter off to the U.S.; however, for me, it was a new adventure.
Did you encounter any obstacles on your path to becoming a surgeon?
I attended the University of Mississippi for my undergraduate studies. There were many instances where people said, “Perhaps you should consider something else — nursing, dentistry, nutrition, pharmacy…” You name it. I was told point blank numerous times that it was “very hard to get into medical school,” especially as an international student, and that I should consider another career path. There was also the unspoken reality about my race — despite 12% of the student population being Black, there were only a handful of Black pre-meds in my class.
I was confident that I would succeed. Growing up in Nigeria where everyone looked like me and having a father who was also a surgeon, it never crossed my mind that I could not do it. I immigrated to America to become a doctor and nothing could stand in my way. So off I went on my quest of getting into medical school. With a laser focus on excellence, I graduated magna cum laude, valedictorian of the Honors college, and with multiple scholarship offers to top medical schools throughout the country.
I chose to attend the University of Chicago where, of the 104 medical students in my class, only 12 of us were Black. Although we were minorities underrepresented in medicine, we were powerful. Of those 12 Black medical students, six of us, five of whom were women, went into surgical specialties.
Do you think your father’s profession influenced you at all?
Absolutely. The surgical persona is one where you get things done; you make a decision, and you go for it. My dad never talked about work at home, but I believe that on a subconscious level — seeing that sort of decisiveness in my father — influenced me.
Why did you choose cardiovascular medicine — specifically cardiac surgery?
I had a lot of exposure in medical school to surgical oncology and most of my mentors were surgical oncologists. Thus, I started general surgery residency with the belief that I was going to become a surgical oncologist.
During my research years in residency, I had the opportunity to train at the National Institutes of Health for a surgical oncology research fellowship. While there, I worked with a thoracic surgeon and experienced the full spectrum of cardiothoracic patient care — from the clinic to the operating room to post-operative care to discharge and back to clinic. At the conclusion of my research fellowship, I transitioned into the 4+3 integrated cardiothoracic surgery program at the University of Washington.
It was a tough decision choosing between cardiac and thoracic surgery. While a lot of people remain undifferentiated as cardiothoracic surgeons, I knew that if I wanted to stay in academia, I had to focus on one. Ultimately, I thought to myself, “If I get paged at two o’clock in the morning, what would I like to be woken up for?” And the answer was cardiac surgery.
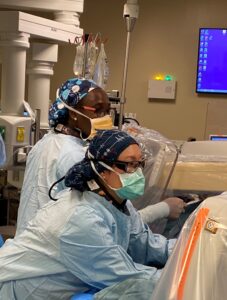
Drs. Lara Oyetunji (back) and Christine Chung (front) during a surgery.
You did your residency at the University of Washington. Today you practice at UW Medicine and at the VA. What kept you here?
The people. I go into the operating room and my day is filled with people that I enjoy working with, from the OR nurses to the ICU team.
I believe that the multidisciplinary heart team approach in the diagnosis and management of cardiac pathology is integral to providing the best care for patients. To a carpenter with a hammer, everything looks like a nail. When you send patients to surgeons, we think, “How can I fix this surgically?”
However, with the multidisciplinary heart team conferences we hold with our cardiology and cardiac anesthesiology colleagues, we are able to think outside the box to come up with the most optimal treatment approach. The sense of community within the Cardiac Surgery team and Heart Institute is strong. It’s a very dynamic and collaborative group here at UW and at the VA.
What would you like to see in the future of cardiovascular care?
Approximately 5% of practicing physicians in the U.S. are Black. Less than 3% of cardiologists and cardiothoracic surgeons are Black. Yet, African Americans have the highest prevalence of cardiovascular disease — hypertension, hyperlipidemia, high cholesterol, obesity, coronary artery disease. And, we also have the poorest clinical outcomes. I think one major way we can truly do right by our patients is to create a more representative workforce that can appropriately address the needs of these at-risk populations.
How do we encourage more diversity?
Get underrepresented minorities interested in science at an early age to help feed the pipeline. There are several nonprofit groups where the goal is to expose minority students to the healthcare profession. Estell J. Williams, MD, is the executive director of Doctor For A Day — an outreach program through the UW School of Medicine which provides underserved K-12 students in the Seattle and Greater Seattle area exposure to medicine and surgery.
Dr. Williams brings students as young as 6 for educational sessions. During our sessions they interact with a beating heart simulator, explore the anatomy of a pig heart, intubate a “patient” and discuss cardiovascular risk factors in different communities. The program helps plant that initial seed that they can be healthcare professionals.
There are many challenges that accompany this profession, but it starts with believing in yourself first. It does not matter if people tell you that you can do it. If you don’t believe it, if you don’t see yourself in that role, then it becomes exceedingly more challenging to make it happen.
As a trailblazer, assistant professor, section chief and cardiothoracic surgeon, what other roles do you see yourself in?
For me, it’s not enough to do well in the U.S. — it’s not enough for me to come to work, take care of patients, go home and be comfortable. My success in the U.S. is a stark reminder of the ongoing brain drain from African countries to western countries, and giving back in a significant way is important to me.
The burden of cardiovascular disease outside of the U.S. is quite high and access to cardiac surgery is essentially nonexistent in low- and middle-income countries, especially in sub-Saharan Africa. To effectively make an impact in global surgery, I felt it was important to learn a different skill set than that which I learned in my medical education. I took a year off between my residency and fellowship to get my master’s degree in public health at Johns Hopkins University. One of my goals is to combine all my experiences to help develop academic twinning partnerships in low- and middle-income countries with the hope of establishing cardiac surgery collaboratives in sub-Saharan Africa. To make a difference in this space, we need to reframe the narrative and consider cardiac surgery as a necessity, and not a luxury.
This article was originally published on Doximity.com.


