Highlights | The future of the operating room (OR)
- Hybrid ORs, robotic techniques and more minimally invasive procedures are replacing traditional surgery.
- Many of these procedures take less time and patients recover faster.
- Many heart conditions, such as aortic and mitral valve abnormalities, can be treated this way now.
- In October of this year, UW Medical Center – Montlake will begin a new fetal surgical program.
- These changes offer numerous unique opportunities for nurses to develop their careers.
Technology and best practices are always advancing in medicine, and there are few places where this is more apparent than in the field of surgery.
The team at UW Medical Center – Montlake is helping bring these new technologies to patients.
The future of surgery
What we have previously called surgery is changing so much that many of the most recent advances are being performed outside of the OR and in procedural areas, says Carla Brannen, assistant administrator of Surgical Services.
These are areas where doctors (aka proceduralists) and nursing and technician teams perform procedures that are more invasive than a standard outpatient appointment but much less invasive than traditional surgery.
One of these areas is a hybrid OR, which allows for a myriad of less-invasive procedures and more sophisticated imaging techniques. Many procedures may only require local anesthetics and moderate sedation, Brannen says. In these spaces both surgeons and proceduralists may work alongside each other or independently.
“One day a surgeon and their team may be using it as a more traditional OR and the next day there might be a cardiologist or interventional radiologist using it,” Brannen says.
And these changes aren’t just happening for surgeons.
“Anesthesiologists used to spend all of their time in the OR, but now may spend up to 40% of their time in procedural sites assisting radiologists, cardiologists, gastroenterologists and other providers rendering care to these patients. It’s a very different world,” says Brannen.
Minimally invasive heart procedures
The Structural Heart Program at the UW Medicine Heart Institute, while being one of the top programs in the country, is one of the programs where these new procedures happen on a routine basis.
Instead of surgeries that involve opening the chest, doctors are now are able to make a small incision and to place a loaded catheter through an artery in the leg or arm to reach the heart. Specially trained nurses work closely with the cardiologist to facilitate appropriate deployment of these devices.
This technique can be used to restore function to a faulty aortic valve, mitral valve and prevent large blood clots from forming in people who have atrial fibrillation.
“Within 20 years we’ve gone from very invasive procedures associated with a significant mortality rate and long hospital stay to procedures where people may actually go home the same day,” Brannen says.
New and expanding surgical programs
Brannen and colleagues have been assisting with the expansion of UW Medical Center – Montlake’s robotic surgery program, too. The hospital now has five robots, each of which performs procedures in a different way.
One of the new robots allows complex surgery of the head and neck to be performed through a single port. While robotic surgery may take more time compared to traditional surgeries, because it is less invasive and less tissue damage occurs due to the precision offered by the robot, patients experience profoundly less pain and much faster recovery.
Nurses play a significant role in the preparation and process of these complicated procedures, Brannen says, because the surgeon is generally not immediately at the bedside because they are operating from the robot console in the periphery of the OR.
Beginning in October, Brannen and colleagues will be collaborating with doctors at Seattle Children’s to offer a new fetal surgical program. Fetal surgery takes place when a fetus is still in the womb. It is an emerging area of surgery and, clearly, takes delicacy to perform.
The program will start by providing fetoscopic laser surgery for twin-twin transfusion syndrome. This is a procedure that becomes necessary when one twin is receiving more blood flow than the other when sharing one placenta. To make sure the other twin doesn’t lose access to blood flow, doctors use a laser to carefully diminish the excessive flow to the one twin and divert it to the other.
The program expects to grow and perform more complex fetal surgeries with time.
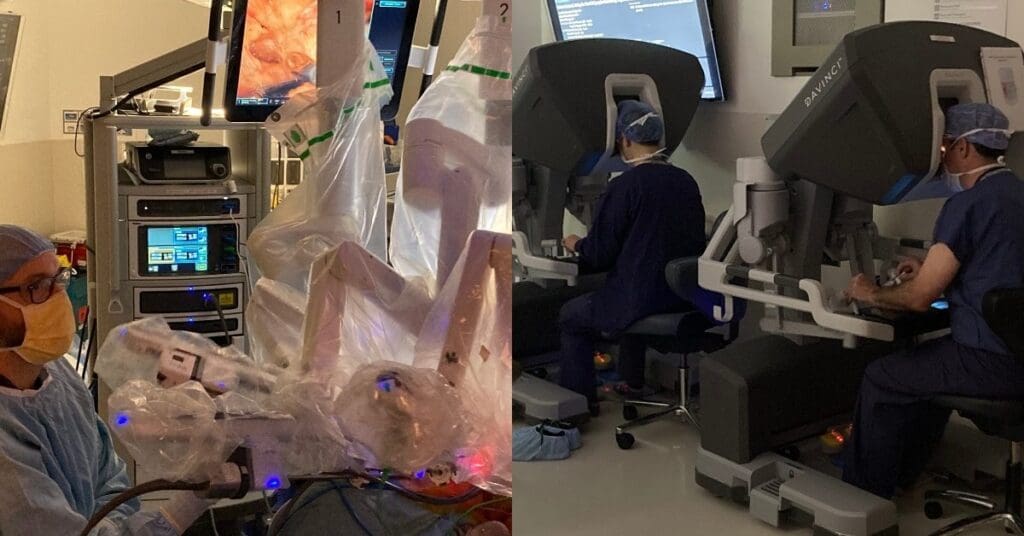
The Urological surgery team at UW Medical Center – Montlake performing robotic surgery on a patient. Note the numerous arms of the robot and that the surgeons are actually performing the operation while sitting at consoles away from the patient.
Many benefits for patients
One of the biggest benefits of hybrid OR technology and other minimally invasive techniques is that the recovery time is much shorter for patients, Brannen says. Procedures that used to be risky, take all day and require long periods of recovery are now safer, take only a few hours and don’t usually require much in-hospital recovery. Also, patients that were previously not deemed surgical candidates may now be eligible for these procedures.
Additionally, all patients receiving surgical care in the UW Medicine system are assisted by “Enhanced Recovery After Surgery” protocols that include elements of the latest clinical evidence to improve a patient’s outcome.
Patients seeking care at UW Medical Center – Montlake are amongst the most complex in the country. Brannen and her team want patients to know that not only are they getting the best, safest medical care, but that operative team is also truly focused on their well-being.
“During my 29 years of surgical nursing, there has never been a more exciting time to be working in the OR. We feel at UW Medical Center that the role of the nurse is expanding to help develop innovative and create solutions for our patients and physician partners. OR nursing also maximizes the use of highly sought after talents such as technology management, communication skills and advocacy for patients and our physician partners,” says Brannen.