Data Snapshot
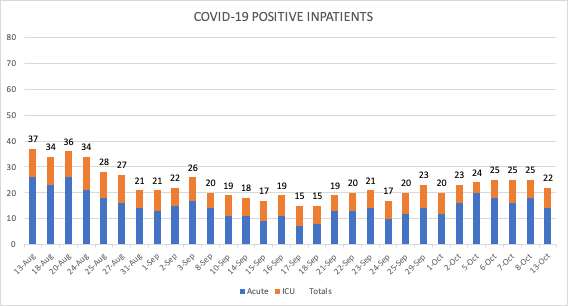
UW Medicine Hospitals:
King County: The county reported 152 new positive cases and 0 new death on Oct. 12.
Washington: The state reported 93,035 cases and 2,910 deaths as of Oct. 9.
United States: The CDC reports 7,740,934 cases and 214,108 deaths as of Oct. 12.
Global: WHO reports 37,601,848 confirmed COVID-19 cases and 1,077,799 deaths as of Oct. 13.
*Numbers update frequently, please follow links for most up-to-date numbers.
COVID-19 Literature Situation Report
COVID-19 Literature Situation Report is a daily (M-F) newsletter put together by the Alliance for Pandemic Preparedness that provides a succinct summary of the latest scientific literature related to the COVID-19 pandemic.
Key Takeaways: COVID-19 Literature Situation Report Oct. 9, 2020
- Children with asthma or obesity who were hospitalized with SARS-CoV-2 were at increased risk for critical care admission or need for respiratory support. More.
- Two thirds of adults with non-critical COVID-19 in an observational study had persistent symptoms up to 2 months after initial symptom onset, including loss of taste or smell, difficulty breathing, or fatigue. More.
- COVID-19 attributable mortality in patients with pre-existing cancer was associated with older age, a higher Charlson comorbidity score, and certain types of cancer. More.
- A study of children infected with SARS-CoV-2 indicated that among children for whom the source of infection was identified, 74% were infected by a member of their household. More.
UW Medicine in the News
KING 5: Puget Sound health experts share what they’ve learned since the COVID-19 pandemic hit
Featuring: Jeffrey Duchin, Allergy & Infectious Diseases; Ali Mokdad, IHME
“Dr. Jeffrey Duchin, Health Officer, Public Health Seattle – King County: ‘An important early lesson is that alignment of elected leaders and public health and medical experts allowed a rapid and effective response to the initial COVID-19 outbreak through community mitigation measures including the stay-at-home order, limiting public gatherings and non-essential activities, and face mask requirements.’”
“Dr. Ali Mokdad, Professor, Health Metrics Sciences – University of Washington: ‘I have been surprised by the lack of a nationally coordinated response to the pandemic. A lack of strong coordination at the national level has led to patchwork responses across states and very different situations in different states.’”
Modern Healthcare: What we’ve learned; Even the brightest and most-prepared hospital CEOs couldn’t have been ready for the initial wave of COVID-19, but now they’ve learned a few things
Featuring: Paul Ramsey, CEO, UW Medicine
“Real-time data on COVID-19 admissions in emergency departments, information on positive coronavirus tests across the system, data regarding available supplies and predictive analytics proved essential for Seattle-based UW Medicine as it faced an early surge of COVID-19 cases. Although the academic health system, as the region’s Level 1 trauma center, is accustomed to command center systems, it had little experience using real-time dashboards during a crisis of this magnitude. ‘We recognized really early on this need for central decision making based on good information that is assembled on dashboards and using the data to make projections about where the pandemic might be going,’ said Dr. Paul Ramsey, the system’s CEO. Real-time dashboards have been used in healthcare for some years now, but Ramsey said the pandemic solidified their use going forward. ‘The need to do this so rapidly with COVID was a bit of a stress test, but it allows us to create better systems’ beyond the pandemic, he said.”
KIRO 7: Concerns over rapid test effectiveness for UW Football after NFL COVID-19 outbreak
Featuring: Geoffrey Baird, Laboratory Medicine, Jeffrey Duchin, Allergy & Infectious Diseases
“UW Medicine’s Dr. Geoffrey Baird explains one of the downsides of rapid antigen tests. ‘All of those tests have a serious decrement in their sensitivity, and yes – allow people who have the virus on board to get passed with a negative result,’ Baird said. It means the rapid tests are just not as good in catching the virus in people with no symptoms. ‘Eventually the virus load goes up and up and up, and eventually gets up to a point where you can detect it. But in a specific case it doesn’t help you,’ Baird said.
Public Health Officer Dr. Jeff Duchin said some antigen tests can also show false positives. ‘In populations that are highly likely to have COVID-19 in an outbreak setting where people are symptomatic, a positive test is relatively reliable. But in screening with people who have no symptoms or not known to be exposed, a positive test has a high likelihood of being a false positive test. That should be confirmed with a PCR test,’ Duchin said during a Zoom conference this week.
Coach Lake says those are concerns they’re very aware of, which is why all players also get those PCR (polymerase chain reaction) tests. PCR tests are slower because they need to go to a lab for results, but it’s what public health calls the ‘gold standard’ of COVID-19 testing.”
Tweet of the Week
A new research preprint estimates that when an infected person and a non-infected person both wear masks, chance of transmission drops by up to 80% vs a scenario where neither is masked. Joshua Schiffer, researcher @UWMedicine co-author. @TheAtlantic https://t.co/icETrizOv5
— UW Medicine Newsroom (@uwmnewsroom) October 13, 2020
